[fusion_builder_container hundred_percent=”no” equal_height_columns=”no” menu_anchor=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” background_color=”” background_image=”” background_position=”center center” background_repeat=”no-repeat” fade=”no” background_parallax=”none” parallax_speed=”0.3″ video_mp4=”” video_webm=”” video_ogv=”” video_url=”” video_aspect_ratio=”16:9″ video_loop=”yes” video_mute=”yes” overlay_color=”” video_preview_image=”” border_color=”” border_style=”solid” padding_top=”” padding_bottom=”” padding_left=”” padding_right=”” type=”flex”][fusion_builder_row][fusion_builder_column type=”1_1″ layout=”1_1″ background_position=”left top” background_color=”” border_color=”” border_style=”solid” border_position=”all” spacing=”yes” background_image=”” background_repeat=”no-repeat” padding_top=”” padding_right=”” padding_bottom=”” padding_left=”” margin_top=”0px” margin_bottom=”0px” class=”” id=”” animation_type=”” animation_speed=”0.3″ animation_direction=”left” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” center_content=”no” last=”true” min_height=”” hover_type=”none” link=”” border_sizes_top=”” border_sizes_bottom=”” border_sizes_left=”” border_sizes_right=”” first=”true”][fusion_text]
Follow @mila_mirceta
[/fusion_text][/fusion_builder_column][/fusion_builder_row][/fusion_builder_container][fusion_builder_container hundred_percent=”no” equal_height_columns=”no” menu_anchor=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” background_color=”” background_image=”” background_position=”center center” background_repeat=”no-repeat” fade=”no” background_parallax=”none” parallax_speed=”0.3″ video_mp4=”” video_webm=”” video_ogv=”” video_url=”” video_aspect_ratio=”16:9″ video_loop=”yes” video_mute=”yes” overlay_color=”” video_preview_image=”” border_color=”” border_style=”solid” padding_top=”” padding_bottom=”” padding_left=”” padding_right=”” type=”flex”][fusion_builder_row][fusion_builder_column type=”1_1″ layout=”1_1″ background_position=”left top” background_color=”” border_color=”” border_style=”solid” border_position=”all” spacing=”yes” background_image=”” background_repeat=”no-repeat” padding_top=”” padding_right=”” padding_bottom=”” padding_left=”” margin_top=”0px” margin_bottom=”0px” class=”” id=”” animation_type=”” animation_speed=”0.3″ animation_direction=”left” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” center_content=”no” last=”true” min_height=”” hover_type=”none” link=”” border_sizes_top=”” border_sizes_bottom=”” border_sizes_left=”” border_sizes_right=”” first=”true”][fusion_text columns=”” column_min_width=”” column_spacing=”” rule_style=”default” rule_size=”” rule_color=”” content_alignment_medium=”” content_alignment_small=”” content_alignment=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” sticky_display=”normal,sticky” class=”” id=”” font_size=”” fusion_font_family_text_font=”” fusion_font_variant_text_font=”” line_height=”” letter_spacing=”” text_color=”” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=””]
At the onset of the COVID-19 pandemic, I had a glimmer of hope that maybe through this crisis, trust in science and the importance of scientific research would become indisputable. It felt like we would finally see an example of what a world without just ONE vaccine for a deadly infectious disease would look like. But the stories that the world chooses to focus on, and those that are shared across non-expert audiences, tell a different story. A story where the experts have absolutely no idea what they are talking about and are continuously contradicting one another. A story where your Facebook acquaintance who went to Google University ‘was right all along’ and continues to share their toxic conspiracy theories to undermine the global effort against this virus.
The sobering fact is that COVID-19 has officially infected over 36 million people and tallied up >1 million casualties in a mere 9 months1. We know both cases and deaths are being severely underreported around the world. The official number of COVID-19 deaths is drastically lower than the total number of excess deaths this year in most countries (excess is determined by comparing the number of deaths this year against the historical 5-year average per country; see Table below) 2,3,4,5.
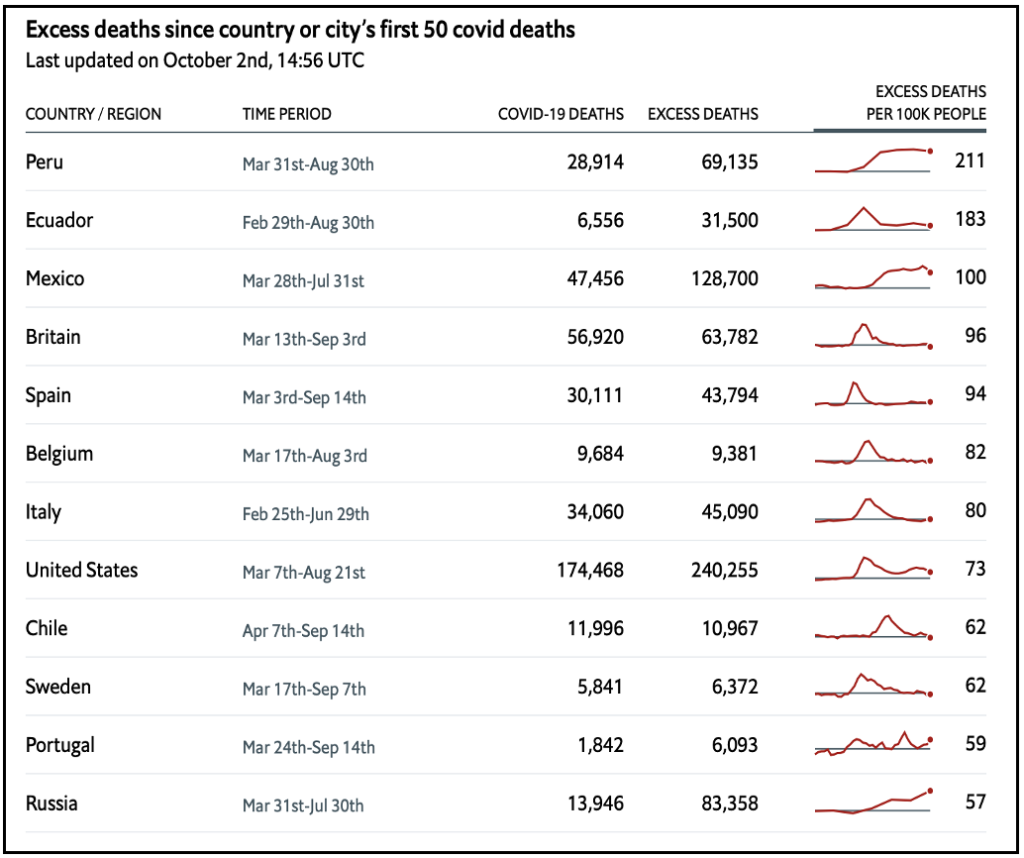
There are many reasons why excess deaths may not necessarily be due to actual infections, but we cannot deny that the majority of them likely are. The data also shows that a surprising number of unusual symptoms – such as neurological symptoms, blood clots and strokes – seem to be associated with COVID-196,7,8. Furthermore, studies are suggesting that production of neutralizing antibodies is both variable and possibly not even as long-lasting as was hoped9,10,11,12. We do not know enough about the disease to make concrete conclusions just yet, but the evidence over the past few months has been quite alarming and attempts to downplay these facts are incredibly counterproductive.
So, why has it been so hard for people to trust the official narrative? I think the past few years have created the perfect breeding grounds for this virus – with rising distrust towards foreign (and domestic) governments and the attack against expertise in this ‘infodemic’. Unfortunately, in the current crisis, official agencies like the WHO and CDC have only added fuel to the fire with inconsistent and poorly explained information. When WHO’s official narrative that ‘masks aren’t necessary against COVID-19’ was changed by the CDC to recommend ‘wearing a home-made face covering in public or when distancing is not possible’ – the credibility of the WHO was shattered. Still today, most people do not understand the data that informed either of these recommendations. The public didn’t understand that the WHO focused on the fact that social distancing makes masks unnecessary, without realizing that in today’s society, distancing is not possible 100% of the time. Also, historical clinical research in hospital settings shows that even properly trained individuals are at higher risk of infection due to improper PPE use13,14,15,16. Just a quick survey of people on the street nowadays shows you that the vast majority are engaging in some kind of contaminating activity. Based on the obvious risks and considerations of wearing masks without proper training, an unclear idea of the infectivity and spread early on, and the looming mask shortage worldwide, a decision was made to tell the public that masks were not helpful. This was not the right way to convey the message. With my obvious hindsight bias, more effort to reliably and transparently share the data and educate the public should have been paramount to maintain their trust as the virus continued to spread. Overall, the last few months have been a public relations nightmare and the experts have looked like they had no idea what they were talking about.
Of course, I’m being incredibly critical of scientists – experts who have spent their lives furthering their respective fields and are not extensively trained on how to effectively communicate to the general public. There is also substantial blame to be placed on the media and their attempts to communicate science in an attention-grabbing manner, without sufficient training in scientific communication. This is why organizations – such as the WHO and CDC, with the help of many grassroots organizations – should be embedding a stronger science communication and literacy campaign within their operations. We, as publicly funded scientists, must also recognize the important role we have in engaging with the people who actually fund our work. Perhaps you may disagree with me, and that I am holding scientists up to a standard that doesn’t fit our job descriptions. Regardless of your willingness to step up as a science advocate, we must all recognize that we at least have a social obligation to ensure we are responsibly sharing our discoveries in a productive and understandable manner. Scientists frequently over-inflate and speculate about the broader significance of their work in scientific publications and grant applications, but this practice is relatively benign when read by other scientific experts who have been trained to critique the science and know that (A) scientists are extremely passionate about their work and (B) this is how we sell the value of our projects. But when we translate our findings to the non-expert public through the media, we need to recognize the greater societal ramifications. We need to take a step back and humbly discuss our exciting findings since the public is not trained in understanding scientific jargon or the way science is done.
In my opinion, there are four important messages we should relay to the general public:
(1) Science is an ever-evolving process. Specifically, one group of scientists makes a discovery that pushes the field an inch forward in a certain direction. In peer review, at least 2-3 experts within that particular field review the work, anonymously to determine whether the conclusions are supported by the data. They request extra experiments/modifications to substantiate the claims and advise if the work is even worthy of publication in the journal. A particular study may start to change the way we think about a particular idea, and other scientists will use those conclusions to make novel hypotheses that further support or refute this idea. As more evidence comes forward, a clearer picture emerges. COVID-19 is incredibly novel, and the current crisis has allowed for the publication of papers that have barely been properly reviewed – with >59 000 papers either published or in pre-print servers over the last 9 months18. Some published papers show a 24-hour timeframe between paper submission and acceptance – a feat we know is impossible in a proper peer review. SARS-CoV-2 research is most definitely the messiest scientific landscape we’ve ever had, and with this all playing out on a global stage, the pressure is high on scientists to show the public that we should be trusted.
(2) Focusing on a single study is never part of the scientific process. A sea of data from independent groups around the world builds the paradigm within a particular field. And as new studies emerge, we shift ideas and our focus. A paradigm shift is achieved through, what sometimes feels like a painstakingly, slow process. Explaining that it is incredibly rare that some radical ‘mind-blowing’ study will destroy the current paradigm is crucial. Or that some whistleblower in the vast network of publicly funded research is being silenced from releasing their scientific data is absolutely preposterous. Every scientist is skeptical to believe the work of a single study until future studies validate and expand on their studies. This is even more true now in the current COVID-19 crisis. No single study is the be-all end-all of a discussion in any scientific field. So why do we let the media report it as such?
(3) Science is not perfect. Mistakes are made accidentally, and there are bad players just like in any discipline. We know that the scientific process will weed out the overwhelming majority of this. This may happen in peer-review prior to publication. Or it will happen as a retraction, such as the Surgisphere scandal19, another polarizing scandal related to hydroxychloroquine, that may seem like another blow to science. But really, it also serves as proof that the scientific community can self-correct relatively quickly and that those ‘checks and balances’ in scientific discovery really do work. Even examples like the falsified and subsequently retracted work from Dr. Andrew Wakefield, claiming to show that vaccines cause autism, has its value. At least now, after 20 years of countless research groups wasting millions upon millions of funding on this question, we can actually definitively say that we know there’s no link between vaccines and autism. The question still remains: how do we convince the public?
(4) Accountability and transparency are core scientific principles. The scientific community is vast and impossible to silence – across both public and private institutions. The demand for transparent and comprehensive data from the experts for independent review will always exist. Debates about the limitations of emerging COVID-19 data, as well as criticism of the controversial actions of the FDA or CDC are continuously occurring amongst experts. This is taking place through official scientific forums, but also within the media and the very public realms of science Twitter and Reddit. The scientific community has been incredibly vocal against the two emergency use authorizations (EUAs) of both hydroxychloroquine and convalescent plasma therapy, because in both instances concrete data in support of their use does not yet exist. Now, with overwhelming data showing hydroxychloroquine is both dangerous and ineffective at reducing COVID-19 severity and mortality20, the EUA has been rescinded. These premature authorizations by the FDA are inexcusable, but also serve as evidence that the vast scientific community is holding these agencies accountable to make evidence-based decisions. The same can be said about vaccine approval, with most scientists expecting full access to the clinical trial data before FDA-approval.
Consequently, scientists are dismissing conspiracy theories, not because we are being silenced by our institutions against ‘speaking the truth’, but because what is being proposed by non-experts is completely illogical. Theories involving so-called COVID-19 patents filed years ago, microchipping by Bill Gates or 5G technology continue to emerge and spread like wildfire, making it increasingly difficult to explain why each theory is incorrect. Rather, what needs to be emphasized is that when true scientific concerns or debates about data exist, the scientific community does mobilize and act to address the injustice. This discourse is typically not as accessible to the public, and because of the lack of understanding in the scientific process, the public can be easily swayed by conspiracy theories that seem logical to them as outsiders. If we continue to try to extinguish each new conspiracy theory individually, we will never win the trust of the public during this Infodemic.
A new strategy is necessary – one that is centred upon explaining that millions of scientists around the world make up the many government scientific agencies (NIH, NIAID, Health Canada, European Medicines Agency, WHO, etc), professional associations and societies, university and hospital scientific networks, and privately funded institutions. All of these scientists – and especially the thousands of experts within a particular field – have access to the complete scientific research and clinical data to independently evaluate the work. A consensus across most scientists and medical professionals is achieved through independent thought and the continuous collection of supporting data. Scientific consensus is not static and can change due to new evidence, but such shifts never come from a single so-called ‘whistleblower’ because the idea of silencing so many experts across all these various institutions is just preposterous.
Overall, I believe if we can learn to more effectively explain the nature of the scientific process, we will regain the public’s trust in medicine and science. I am not arguing that the scientific process is infallible, but that the oversight from the scientific community gives incredible trustworthiness to the process. As scientists and medical professionals, we need to do our best to responsibly and frequently engage with the non-experts in our everyday lives. Be a voice of trust and take an open and communicative approach to sharing facts and directing people to trustworthy resources. Importantly, for your own sanity, know when to quit because there will be many people resistant to being wrong, and there’s nothing you can do. This is a tall order for us to fill, but something we should all strive for – because really at its core, public health demands that we first care about others in order to ultimately care about ourselves. And no, I don’t think this will solve all the problems, but it’s a worthy start.
References
- 1. Worldometers.info. 2020. Coronavirus Update (Live): COVID-19 Virus Pandemic – Worldometer. [online] Available at: this link [Accessed 28 June 2020].
- 2. The Economist. 2020. Tracking Covid-19 Excess Deaths Across Countries. [online] Available at: this link [Accessed 28 June 2020].
- 3. Financial Times. 2020. Coronavirus Tracked: The Latest Figures As Countries Start To Reopen [online] Available at: this link [Accessed 28 June 2020].
- 4. New York Times. 2020. 120,000 Missing Deaths: Tracking The True Toll Of The Coronavirus Outbreak. [online] Available at: this link [Accessed 28 June 2020].
- 5. BBC News. 2020. What Is The True Death Toll Of The Coronavirus Pandemic?. [online] Available at: this link [Accessed 28 June 2020].
- 6. Wadman M, et al. 2020. How Does Coronavirus Kill? Clinicians Trace A Ferocious Rampage Through The Body, From Brain To Toes. Science News. [online] Available at: this link [Accessed 28 June 2020].
- 7. Klok FA, et al. Incidence of thrombotic complications in critically ill ICU patients with COVID-19. Thromb Res. 2020;191:145-147. doi:10.1016/j.thromres.2020.04.013
- 8. Larson AS, et al. Coronavirus Disease 2019 and the Cerebrovascular-Cardiovascular Systems: What Do We Know So Far? [published online ahead of print, 2020 May 12]. J Am Heart Assoc. 2020;e016793. doi:10.1161/JAHA.120.016793
- 9. Long Q, et al. Antibody responses to SARS-CoV-2 in patients with COVID-19. Nat Med 26, 845–848 (2020). Available at: this link
- 10. Robbiani DF, et al. Convergent antibody responses to SARS-CoV-2 in convalescent individuals. Nature (2020). Available at: this link
- 11. Long Q, et al. Clinical and immunological assessment of asymptomatic SARS-CoV-2 infections. Nat Med(2020). Available at: this link
- 12. Kirkcaldy RD, King BA, Brooks JT. COVID-19 and Postinfection Immunity: Limited Evidence, Many Remaining Questions. JAMA. 2020;323(22):2245–2246. doi:10.1001/jama.2020.7869
- 13. Tomas ME, et al. Contamination of Health Care Personnel During Removal of Personal Protective Equipment. JAMA Intern Med. 2015;175(12):1904-1910. doi:10.1001/jamainternmed.2015.4535
- 14. Kang J, O’Donnell JM, Colaianne B, Bircher N, Ren D, Smith KJ. Use of personal protective equipment among health care personnel: Results of clinical observations and simulations. Am J Infect Control. 2017;45(1):17-23. doi:10.1016/j.ajic.2016.08.011
- 15. Zellmer C, Van Hoof S, Safdar N. Variation in health care worker removal of personal protective equipment. Am J Infect Control. 2015;43(7):750-751. doi:10.1016/j.ajic.2015.02.005
- 16. Sujan C Reddy, Amy L Valderrama, David T Kuhar, Improving the Use of Personal Protective Equipment: Applying Lessons Learned, Clinical Infectious Diseases, Volume 69, Issue Supplement_3, 1 October 2019, Pages S165–S170, https://doi.org/10.1093/cid/ciz619
- 17. Akst, J., 2020. WHO Comments Breed Confusion Over Asymptomatic Spread Of COVID-19. [online] The Scientist Magazine. Available at: this link [Accessed 28 June 2020].
- 18. Chen Q, Allot A, Lu Z. Keep up with the latest coronavirus research. Nature. 2020;579(7798):193. doi:10.1038/d41586-020-00694-1
- 19. Mehra MR, Ruschitzka F, Patel AN. Retraction-Hydroxychloroquine or chloroquine with or without a macrolide for treatment of COVID-19: a multinational registry analysis [retraction of: Lancet. 2020 May 22;:]. Lancet. 2020;395(10240):1820. doi:10.1016/S0140-6736(20)31324-6
- 20. Elavarasi A, Prasad M, Seth T, et al. Chloroquine and Hydroxychloroquine for the Treatment of COVID-19: a Systematic Review and Meta-analysis [published online ahead of print, 2020 Sep 3]. J Gen Intern Med. 2020;10.1007/s11606-020-06146-w. doi:10.1007/s11606-020-06146-w
[/fusion_text][/fusion_builder_column][/fusion_builder_row][/fusion_builder_container]
